
A 63-year-old male patient presented to the Emergency Department with palpitations.
The initial ECG suggested Supraventricular Tachycardia (SVT), and the patient was treated with 6 mg of Adenosine, which successfully restored sinus rhythm, as confirmed on the monitor.
Shortly after, a post-cardioversion ECG was ordered. However, the nurse urgently returned with this bizarre-looking ECG.
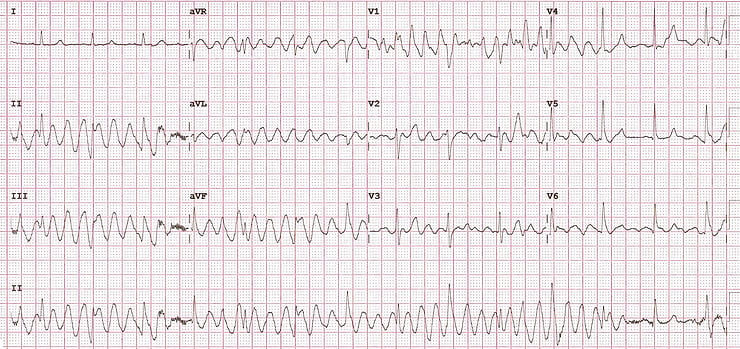
What is your diagnosis and management plan?
Understanding the ECG Anomaly
This ECG offers a perfect teaching moment to revisit a basic principle of ECG interpretation, especially useful for beginners.
Time and the ECG Grid
“When you move horizontally across the ECG paper, you're moving through time. When you move vertically, time is frozen.”
In simpler terms:
Any vertical line (up or down) on the ECG represents the same moment in time across all leads.Applying the Rule
Let’s test this principle using the patient's ECG:
In lead I, the rhythm appears to be normal sinus.
In leads II and III, it looks like polymorphic ventricular tachycardia (VT).
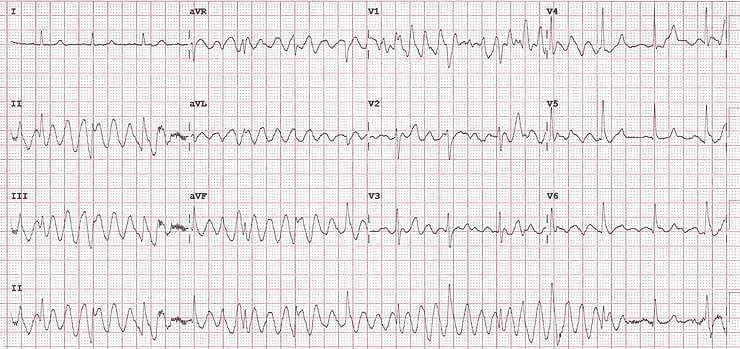
If this were truly polymorphic VT, we'd expect it to progress horizontally with time. But if lead I shows normal rhythm at the same vertical point as VT-like activity in II and III, something doesn't add up.
The Logical Conclusion (H3)
This ECG does not show real VT. Instead, it shows:
Movement Artifacts
By tracing the ECG vertically, you can clearly separate true cardiac complexes from the artifactual waveforms. Horizontally, you’ll also notice a consistent and regular rhythm, which confirms sinus activity.
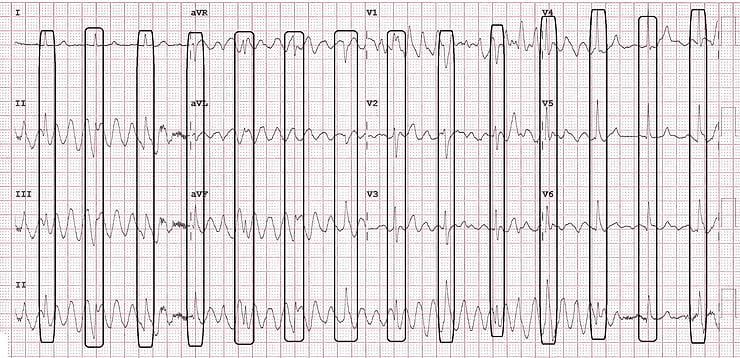
Cause of the Artifacts
This patient was experiencing shivering episodes, likely due to mild hypothermia, which led to the motion-induced distortions in the ECG.
Once rewarmed, repeat ECGs were completely normal.
Another Example of Artifact Mimicking VT
Here’s another case demonstrating movement artifacts mimicking ventricular tachycardia.
Apply the same rule:
Check for rhythm consistency across leads
Follow vertical alignment to detect real vs. false signals
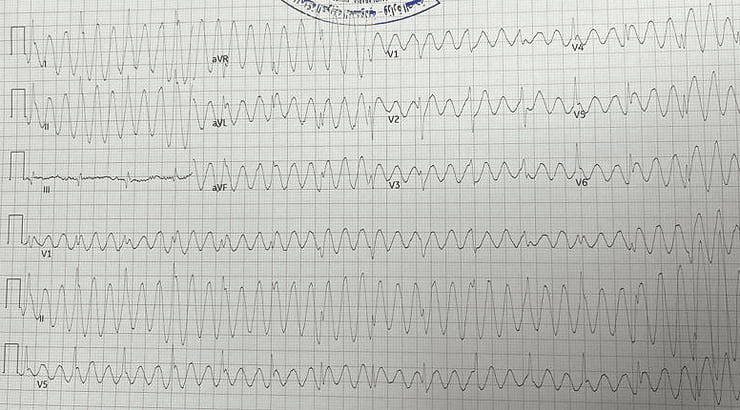
Example courtesy of Dr. Anas Halim, Emergency Physician, KSA
Key Takeaways
Always consider movement artifacts when ECGs show conflicting lead findings.
Remember: vertical = same moment in time. Use this to expose inconsistencies.
Reassess and repeat the ECG after stabilizing the patient, especially if they’re shivering or hypothermic.
Next time you see a strange ECG like this, ask yourself: “Should I really worry about this rhythm?”
✅ Final FAQ Section
Q1: How can you differentiate movement artifacts from ventricular tachycardia on an ECG?
A1: By checking the vertical alignment: real electrical activity remains consistent across leads, while artifacts cause irregularities that don’t match simultaneously across leads.
Q2: What causes movement artifacts in ECG recordings?
A2: Movement artifacts can result from patient shivering, tremors, loose electrodes, or motion during recording, mimicking arrhythmias like ventricular tachycardia.
Q3: Why is it critical to identify movement artifacts early?
A3: Misinterpreting artifacts can lead to incorrect diagnosis, unnecessary treatments, and patient anxiety; correct interpretation ensures appropriate management.
🔗 Further Learning
Watch a detailed case breakdown on YouTube:
▶️ Video: ECG Movement Artifact vs VT - YouTube
